Indiana HIV Outbreak 2015: Cases Rise To 142, Vast Majority Linked To Injecting Prescription Drugs
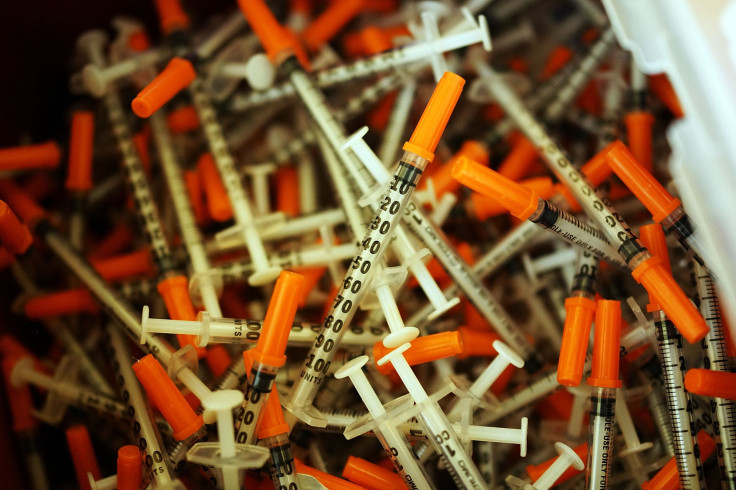
The number of HIV cases in Indiana has risen to 142, health officials said Friday, as state and federal public health officials scramble to contain an ongoing and unprecedented outbreak of the virus in two counties. The vast majority of the cases have been linked to the injection of prescription painkillers, which is part of a growing nationwide problem of prescription drug abuse.
“This outbreak that we’re seeing in Indiana is really the tip of an iceberg of a drug abuse problem that we see in the United States,” Dr. Jonathan Mermin, director of the National Center for HIV/AIDS, said in a call with reporters Friday. He noted that this was the first major outbreak of HIV that had been linked to injecting prescription opioid drugs.
Of 112 people interviewed in a recent investigation by the Indiana State Department of Health, 108 of them, or 96 percent, admitted to injecting drugs. Of the 108, all said they had used the opioid oxymorphone, which goes by the brand name Opana.
Prescriptions for opioid painkillers have skyrocketed in recent years, leading to more abuse of the drugs and, in turn, more infections. In rural and impoverished Scott County, where most cases have been reported, the unique characteristics of a highly addictive drug helped foster the outbreak, particularly in the absence of adequate preventive public health measures.
Oxymorphone is a powerful painkiller that users inject after crushing up the pill and mixing it with water. Sharing needles for oxymorphone carries a higher risk of passing along diseases than for a drug like heroin, because the pill doesn’t dissolve as finely and so larger needles have to be used, increasing the risk of sharing blood and thus diseases, Dr. Jerome Adams, the Indiana state health commissioner, said.
Users also tend to inject the drug frequently, because the effects from oxymorphone last just about four hours, Dr. Joan Duwve, the chief medical consultant at the Indiana State Department of Health, pointed out. “We have heard that folks are injecting from four to over 10 times a day,” she said. Users will go into withdrawal after about four hours, and if they’re with someone else when the cravings set in, they’ll share needles to get another dose.
One reason drug users may be less attuned to the risks of sharing needles is because of their location. In some urban settings, residents might be bombarded with information about why they should not share needles. But in rural areas, “some people might not have received the type of HIV prevention counseling that others have,” Mermin said. Prior to the outbreak, the area hardest hit had just one doctor, who was not an infectious diseases specialist, according to Duwve. Now, there's a weekly clinic to treat HIV.
Demographics also could play a role. Most of the people infected in the current outbreak are young, perhaps too young to remember the devastation of the HIV/AIDS epidemic. “They haven’t been around during the 1980s and early '90s, when HIV was at its peak,” Mermin said.
“We all pay the price when we don’t sufficiently invest in public health, and I think this is an example,” Adams, the state health commissioner, said. He added that the state was working on accruing more funding to continue its response to the outbreak and enhance measures that would make it sustainable.
© Copyright IBTimes 2024. All rights reserved.












