Obama's Healthcare.gov Website Isn't Consumer-Friendly Enough, Experts Say
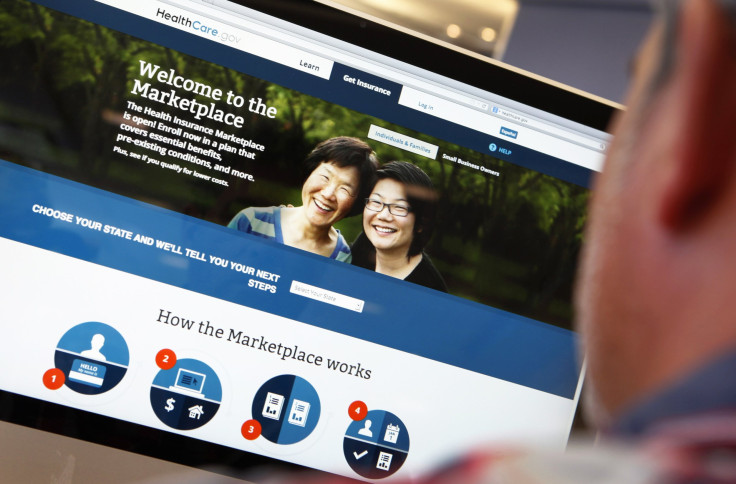
Comparing health insurance plans – whether signing up through Healthcare.gov or weighing employer-sponsored plans with a spouse – can feel like wading through a sea of information on deductibles, co-payments and monthly premiums. Now that more than 11 million people have chosen a plan during this year’s Healthcare.gov enrollment period, which ended on Feb. 15, three experts are pondering how to make this intimidating task even easier for next year’s registrants? They have laid out their prescription for improving the health insurance marketplace, grounded in psychology and behavioral research, in a perspective published Wednesday in the New England Journal of Medicine.
“This is a really complicated decision to make and a pretty high-stakes one, too -- it can mean a lot of money,” Peter Ubel, a co-author and health marketing expert at Duke University, says. “I think a better designed system would actually be faster to go through and yet still help you make a better decision.”
In the existing marketplace, the authors don’t like the way plans are sorted into gold, silver and bronze categories.They think these labels make the gold plans inherently more desirable. The team did a preliminary test of this theory by presenting a choice of two plans to public bus riders in North Carolina – one offering lower monthly premiums but higher out-of-pocket costs than the other – and alternately labeled them “gold” and “bronze.” Inevitably, more than half of riders chose the “gold” plan, no matter if it had the higher or lower premiums and deductibles.
These subtle cues inherent in the labels and layout of the current marketplace may prompt consumers to make a decision that is not in their best interests. “Now that we've made health insurance accessible in a legal sense, we have to make it accessible in a behavioral sense,” Douglas Hough, a health economist at Johns Hopkins School of Public Health who was not involved in the research, says.
Another issue: Many state exchanges rank plans by monthly premium and list the plans with the lowest monthly premiums at the top. Ubel and his co-authors, who include a behavioral scientist from the University of Stirling in the U.K. and a business professor from Columbia University, say this strategy could cause a disproportionate number of people to choose the first plan, citing research that shows a tendency for consumers to choose the wine that is listed first on a curated menu. Arranging plans by deductibles or the number of doctors and hospitals covered may prompt consumers to pick plans in an entirely different pattern, a theory that Ubel says should be tested.
Hough thinks the health insurance marketplace software should play a more active role in aiding consumer decisions by offering suggestions based on their searches or the way other registrants have acted. “Given the complexity, I think people are looking for heuristics, rules of thumb -- they're looking for a guide,” he says. His vision would look more like Amazon.com. “People who bought this have also bought that, people who looked at this have also looked at that,” he says. Or, the interface might work like TurboTax in asking a series of simple questions meant to steer consumers in the right direction.
Since the early technological woes of the Healthcare.gov rollout have largely been overcome, Ubel hopes the Department of Health and Human Services, as well as the agencies that oversee state exchanges, can finally start to speak with behavioral researchers and apply some of these principles. “I actually talked to a couple of groups when they were designing the exchanges to see if they wanted free consultation,” he says. “I had great preliminary phone calls but they were too busy to get back to me, which I understand.”
Hough cautions that while behavioral scientists may be able to lend some insight into this process, they can’t be expected to provide all the answers. “One of the dangers of behavioral economics is people get really excited for it and start applying it willy-nilly without recognizing that there's a lot of things we don't know,” he says. “We know what the solutions are conceptually, but not really at the ground floor where we really need to make the changes.”
© Copyright IBTimes 2025. All rights reserved.






















