OK Glass, Let's Perform Surgery: How Doctors Are Using The Google Device In The Operating Room
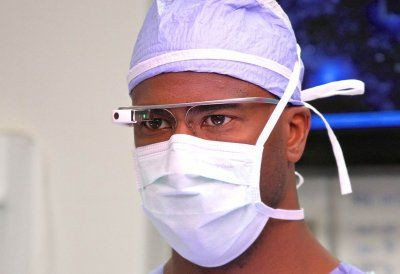
High-tech tools for the operating room: anesthesia machine, heart monitor, and … Google Glass? Yes, some surgeons are donning the wearable computer to see if the device can help doctors better serve patients and educate students.
Now, some students are getting a surgeon’s-eye view of procedures, offering an angle they couldn't see before in the classroom.
"By just winking, the Glass captures an image of whatever you're looking at during surgery," University of Arizona Medical Center surgeon Jason Wild told Tucson television station KVOA. "We've tried using other kinds of cameras, but they require touch control which can be a contamination risk. Glass allows us to capture angles otherwise impossible, to help educate our residents."
Glass isn’t just a boon for teaching purposes; it can provide quick access to vital information that a surgeon needs during an operation. University of California, San Francisco cardiothoracic surgeon Pierre Theodore has found the device useful for taking quick looks at X-ray images during surgery. Without Glass, a doctor usually has to walk over to a display to view film. Even though these interruptions can be brief, in some delicate operations, every second counts.
"Most surgeons will tell you that there have been times when they were not able to access the radiographic images when they needed it," Theodore told Fast Company. "This could potentially compromise an operation."
With Glass, Theodore can preload a CT scan or X-ray image that he’ll need for the procedure, then call up the information right in front of his face when he’s operating on the patient.
“Often one will remove a tumor that may be deeply hidden inside an organ -- the liver, the lung -- for example,” Theodore said in a statement released by UCSF. “To be able to have those X-rays directly in your field [of vision] without having to leave the operating room or to log on to another system elsewhere, or to turn yourself away from the patient in order to divert your attention, is very helpful in terms of maintaining your attention where it should be, which is on the patient 100 percent of the time.”
Other surgeons have had the same idea. A University of Chicago plastic surgeon wore Glass while performing a rhinoplasty on a patient injured at an amusement park this past December; that same month, a University of Alabama-Birmingham orthopedic surgeon shared live video of a shoulder replacement surgery with a colleague in Atlanta, which allowed for real-time virtual consultation between the two physicians.
But the device isn’t perfect: it has a limited battery life, which some surgeons have dealt with by carrying extra battery packs. And the way the device’s camera is positioned isn’t always ideal for capturing photos and videos of surgery. Ohio State University medical student Ryan Blackwell told ABC News that in reviewing videos of surgery, the incisions are sometimes captured near the bottom of the screen and harder to see.
Theodore also ran into some procedural hiccups while trying to integrate the device into his operation. Since Glass runs on Wi-Fi, he had to pick an operating room with the best signal. Since the X-ray images would be traveling over an Internet connection, he had to scrub the X-rays of the patient’s personal information for privacy reasons. And, he told Fast Company, Glass was a little slow to respond correctly to voice commands.
Patients must also consent to their doctors using Glass during procedures (not all people are comfortable with the idea of their insides getting caught on camera). But despite the occasional obstacle, many of the physicians who’ve tried the device are optimistic about its potential.
“If you believe in the fundamental assumption that having accurate data in the hands of the clinician leads to better decision-making, then it would seem to me that having that data in a way that’s convenient, comfortable and always present in the presence of the patient can lead to greater efficiencies and better decision-making overall,” Theodore said.
© Copyright IBTimes 2024. All rights reserved.





















