Emergency 'Triage' Takes On Grim Urgency As Virus Strains Hospitals
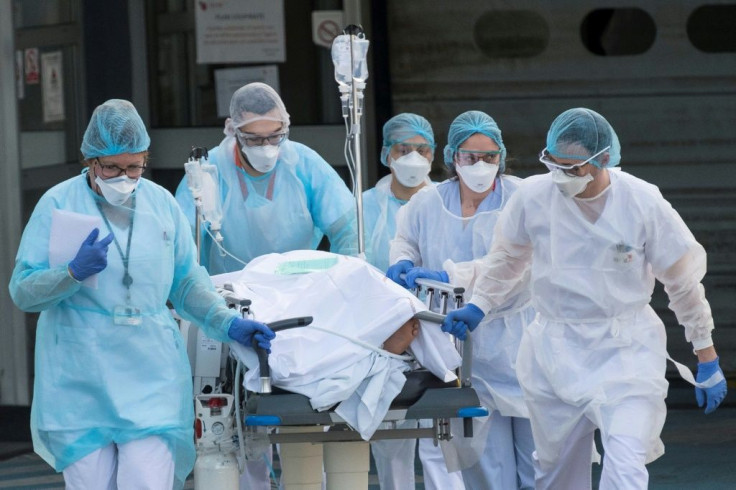
Emergency medics routinely make critical treatment calculations based on their patients' chances of survival.
But as the coronavirus pandemic overwhelms hospitals, physicians are facing the prospect of large-scale triage that some say resembles the stark choices of war.
The virus has infected 300,000 people worldwide and claimed more than 13,000 lives according to official figures, with healthcare systems in the path of the pandemic struggling to cope.
In Italy, the current epicentre of the disease that first emerged in China, medics are already faced with grave choices over which patients to save and other countries are bracing for surging numbers of desperately ill patients.
Many people who catch COVID-19 do not need hospitalisation, but those who develop the most serious symptoms of the respiratory infection can require critical care. But which patients should get a limited number of ventilators?
"Yes, we are going to be called upon to prioritise between the patients," Bertrand Guidet, head of the intensive care unit at Saint-Antoine Hospital in Paris, where the numbers of coronavirus patients have already begun to increase.
"In the words of the (French) president Emmanuel Macron we are at war, and well it's called triage, like on the battlefield where we leave the most gravely wounded because we think they will die," he told AFP.
It is also necessary to maintain capacity over the longer term, said Guidet.
"The patients who present themselves now must not be privileged over those who will arrive in a week or 15 days, we must not saturate everything immediately."
He said that while the current pandemic presents an acute challenge for emergency medics, they do have established guidelines to help them make these decisions.
"We are not starting from scratch, these are decisions we make every day," said Guidet.
Normal evaluation criteria includes "the wishes of the patient", their general state of health and the severity of their symptoms, he said.
Regardless of whether or not there are enough machines, putting the most fragile patients on life-support can be "senseless", experts say.
But in the event of conflict or disaster -- from earthquakes to tsunamis and now coronavirus -- the criteria to decide who is given life support become increasingly strict.
In Italy, where the battle to save as many people as possible has raged for weeks, this is a daily reality for doctors.
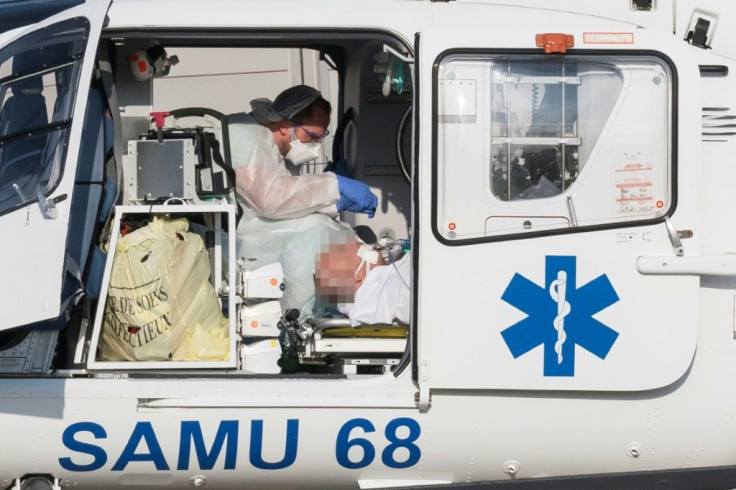
"We're in no condition to attempt what are called miracles. It's reality," Christian Salaroli, an anesthesiologist at the Papa Giovanni XXIII Hospital in Bergamo told the Corriere della Sera newspaper earlier this month.
"I tell myself it's like war surgery... It's decided by age, and health. As in all war situations."
As infections continue to rise relentlessly, frontline health workers across the world are preparing to make similar decisions.
Philippe Devos, an anesthesiologist in Liege, Belgium said in crisis situations respirators are prioritised for those with "the best chance of survival".
"As far as possible, we will try to make sure it is not a lottery," he said, highlighting criteria such as age and the underlying health of the patient.
In early March, as the virus overwhelmed hospitals in Italy's worst hit northern region, the Italian body of anesthesiologists and intensive care professionals, Siaarti, published ethical guidelines that said an age limit for intensive care treatment "may ultimately need to be set".
But age alone is too simplistic a criteria, experts say.
Guidet said he had admitted an 85-year-old patient to intensive care at his Paris hospital who had COVID-19 but had no prior underlying illness and had been completely well before that.
On the other hand, he said there would be no place for someone in their 40s who had severe cirrhosis and continued to drink.
These are the same principles as for organ transplant waiting lists, said Arthur Caplan, director of medical ethics at the New York University Groceman School of Medicine.
"People have been dying every day for decades not getting a transplant," he told AFP.
With the influx of coronavirus patients, the decisions will fall heavily on doctors' shoulders.
"Most hospitals have rules to help the doctors, but in reality, people will not follow rules, the senior doctor will decide, because it's moving too fast," he said.
That is a "huge moral weight" to bear, said Devos.
"We go into medicine to heal people. Not to make choices about who can live."
© Copyright AFP {{Year}}. All rights reserved.



















