Protein That Could Reverse Bone Damage From Osteoporosis Found
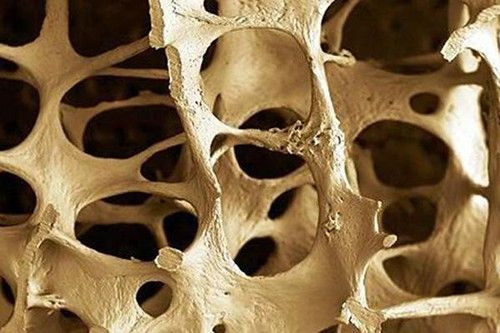
Researchers have identified a pharmaceutical target that could one day make it possible to prevent and roll back damage to bones from osteoporosis.
Despite the stiffness of bone, it is still a living tissue that the body regularly breaks down and replaces. Osteoporosis, which translates from Greek to mean “porous bone”, results when old tissue is lost faster than new tissue it is built, leading to weak and brittle bones. In the U.S., this disease affects over 40 million men and women while being most common in post-menopausal women.
A pharmaceutical target has been identified by biomedical engineers at Duke University that when activated can undo bone degradation due to osteoporosis in mouse models of the disease.
"The most widely used drugs currently approved by the FDA to treat osteoporosis can prevent further bone loss, but they don't help rebuild the bone," said Shyni Varghese, professor of biomedical engineering, mechanical engineering and materials science, and orthopedics at Duke.
"We've discovered a biochemical receptor that, when activated, can do both," added Yu-Ru "Vernon" Shih, a research scientist in Varghese's lab and the study's first author.
In 2014, Varghese was analyzing the function of prominent biomedical devices made of calcium phosphate in encouraging bone repair and regeneration. She found that the biochemical adenosine acting on the A2B receptor has a significant role in encouraging bone growth. It made sense that a reduced amount of the chemical might contribute to the development of osteoporosis, so Varghese set out to investigate this.
In this study, Varghese examined mice that had had their ovaries removed to simulate post-menopausal osteoporosis. They observed the expression levels of two enzymes that play a part in the production of adenosine as well as the levels of adenosine traveling between cells. They found, to their expectations, that the mice’s lack in estrogen was causing the levels of all three drop.
The researchers then sought to see if they could undo the destructive effects of the disease by increasing the adenosine levels. Instead of pumping in adenosine itself, they injected a non-hormonal small molecule produced by Bayer that activates the A2B receptor.
"The mice that received the drug were completely cured," said Varghese. "Their bones were just as healthy as the control group without osteoporosis."
Still, the challenge remains of creating a small molecule drug-specific enough to be free of side-effects. Adenosine is made naturally in the body and serves many functions that include neuron modulation and regulation of blood flow to various organs. Adenosine cannot simply be administered through the blood in an effort against bone degradation without flooding other parts of the body. Molecule specificity is key to minimizing side-effects.
At least with the A2B receptor singled out, Varghese and others can begin researching into ways to deliver activators that bind only to receptors in the bones. For example, one of Varghese's students has commenced methods to tether adenosine-like molecules to carriers that target bone tissue. Her lab is also pursuing a sort of bandage that can convey growth-supporting drugs straight to damaged or broken bones.
© Copyright IBTimes 2025. All rights reserved.





















