MIT Researchers Say New Drug Found May Cure Any Viral Infection
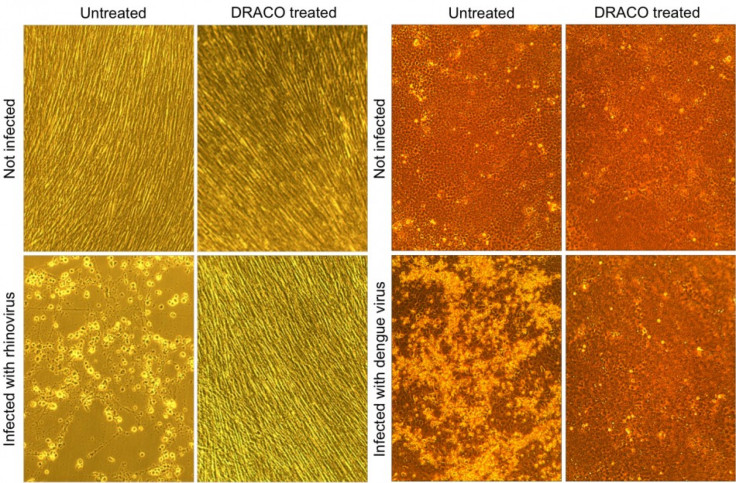
A new drug, dubbed "DRACO," or double-stranded RNA Activated Caspase Oligomerizers, works by targeting a type of RNA produced only in virus-infected cells.
Most bacterial infections can be treated with antibiotics such as penicillin, discovered decades ago.
However, such drugs are useless against viral infections, including influenza, the common cold, and deadly hemorrhagic fevers such as Ebola, according to an MIT news release.
Researchers at the Massachusetts Institute of Technology, or MIT, have developed what could be a groundbreaking drug, which can be read in the journal PLoS One, and seems effective at curing nearly any viral infection to include the common cold, influenza and other such illnesses.
In the paper published July 27 in the journal, the researchers tested their drug against 15 viruses, and found it was effective against all of them — including rhinoviruses that cause the common cold, H1N1 influenza, a stomach virus, a polio virus, dengue fever and several other types of hemorrhagic fever.
The drug works by targeting a type of RNA produced only in cells that have been infected by viruses.
DRACO could potentially be used to fight outbreaks of new viruses, such as the 2003 severe acute respiratory syndrome, or SARS, outbreak, says Todd Rider, who invented the drug.
Rider, a senior staff scientist in MIT's Lincoln Laboratory's Chemical, Biological, and Nanoscale Technologies Group, said, "In theory, it should work against all viruses," in a statement posted on MIT's Web site.
According to a press release on DRACO, Rider had the idea to try and develop a broad-spectrum antiviral therapy some 11 years ago, after inventing Cellular Analysis and Notification of Antigen Risks and Yields, or CANARY, a bio-sensor that can rapidly identify pathogens.
"If you detect a pathogenic bacterium in the environment, there is probably an antibiotic that could be used to treat someone exposed to that, but I realized there are very few treatments out there for viruses," Rider added.
Karla Kirkegaard, professor of microbiology and immunology at Stanford University, says combining those two elements is a "great idea" and a very novel approach.
"Viruses are pretty good at developing resistance to things we try against them, but in this case, it's hard to think of a simple pathway to drug resistance," Kirkegaard said in a statement.
© Copyright IBTimes 2025. All rights reserved.




















