The Patient Is Rubber and She's Talking to You
At 11 a.m. on a Tuesday morning, a 35-year-old woman named Elsie cried out from her hospital bed at Jacobi Medical Center's maternity wing.
The baby's coming, she cried. I'm having contractions!
Two computer screens at the doctors' eye level showed the heart rate of both mother and child, as the competing sounds, one fast and one slow, reverberated through the room over the computer speaker.
Roxanne Connell, the attending obstetrician, could see the baby's head already emerging. Her eyes shifted back and forth from the computer screen to the mother. Something was wrong: The baby's head was emerging and retracting repeatedly, a sign of shoulder dystocia, a dangerous condition in which the baby's shoulders are in a vertical position, lodged against the mother's pubic bone. It may cause suffocation or damage to the baby's neck if not resolved within five minutes.
We are here to help you, Dr. Connell told Elsie. Now please stop pushing.
Dr. Connell tried some internal maneuvers in order to rotate the baby's shoulders into a horizontal position, but they didn't work. Since the baby was lying on its side vertically, Dr. Connell delivered the arm that was under the body first. The delivered arm left more room for the whole body to emerge.
Success. Elsie gave birth to a healthy baby girl two minutes after the problem was detected, well within the five-minute limit.
You did really great! Dr. Connell told Elsie.
Then suddenly, a nurse opened up Elsie's belly and put the baby back in. Stop the simulation, said Jared Kutzin, a simulation educator, to Anil Batra, a simulation specialist who was operating the computer. Reset the birth.
Batra reattached the baby to a magnetic controlling rod inside Elsie's torso. He then clicked on a mini computer that looked like an iPad to move the rod up so that the baby was in an undelivered position again.
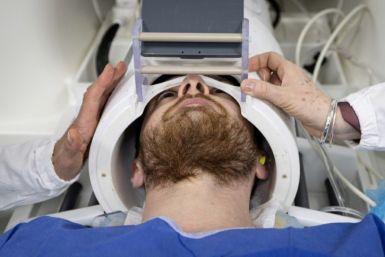
Elsie is a $38,000, high-tech, ultra-realistic simulator made by Gaumard Scientific Company in Miami, Florida, an indispensable tool in the evolving field of medical simulation education. The simulator, whose commercial name is Noelle, is an anatomically correct rubber model of an adult woman's body, embedded with computer chips. The eyes blink, and her pupils react to different levels of light; she also has an electronic pulse. A tiny speaker on the right ear plays the phrases Elsie cried out when she was having contractions.
Elsie's abdomen is a piece of rubber that can be pulled up to examine the internal structure, or attached to the body to simulate a pregnant woman. A computer determines the heart rate and blood pressure of both mother and child, and sends out signals to deliver the baby or create a shoulder dystocia situation.
A plastic capsule about the size of a boxing glove, which contains red ink, can be inserted into the belly to simulate a hemorrhage condition. Surgeons and nurses can also practice C-sections on the simulator.
The unisex baby is simulated too. Its skull demonstrates the natural curves of a real baby. Its hip can be plugged in and out. It cries, breathes and has a pulse. The skin turns blue if he suffers from a shortage of oxygen. Physicians, midwives and nurses can deliver the baby and reattach it as many times as they want.
Elsie and her baby were the central characters in a simulation-training course at Jacobi Hospital's new Institute for Medical Simulation and Advanced Learning, a $10 million, 10, 000 square-foot facility completed in October 2010 by the New York City Health and Hospitals Corporation (HHC).
The first of its kind among public hospital systems in the nation, Jacobi's simulation center employs the latest technology to help improve clinical learning and patient safety at the city's public hospitals.
It's not just a rubber doll, said Dr. Connell, the attending obstetrician from North Central Bronx Hospital who delivered Elsie's baby. It's like the emotional, real-life action.
It is essentially a virtual hospital with 18 simulated patients and a series of partial task simulators that only resemble a body part. Here, doctors and nurses can make mistakes without worrying about hurting anyone, learn from those errors, and practice how to efficiently work together. All of New York City's 11 public hospitals belonging to HHC are entitled to schedule classes here for their employees.
To make the communication part of the training more successful, the simulation center's directors may play the patient's distraught family members, while physicians and nurses practice as a team saving a person's life and consoling loved ones. In this case, it is a hybrid simulation.
On-the-job training is not the only use for medical simulation. At St. Barnabas Hospital in the Bronx, a private hospital that does not belong to HHC, it is used to help select candidates for the general surgery residency program.
For decades, the military and the aviation industry have used simulation to select and train their personnel. In 2007, the Veterans Administration Medical Center in Manhattan started using simulation technology to treat Iraq War veterans with post-traumatic stress disorder.
Medical schools and teaching hospitals, on the other hand, have adhered to the age-old practice of teaching through the observation of experienced doctors in action and the treatment of real patients, a practice that limits training possibilities and exposes both patients and health care providers to preventable risks.
The problems in the health care system today are shorter hospital stays and inadequate insurance, said Anthony Errichetti, PhD, chief of virtual medicine at the New York College of Osteopathic Medicine. So patients may not be there when a doctor wants to teach a particular class. Medical simulation fills this gap by providing educators with more opportunities to teach.
When Kutzin, DPN, director of nursing and clinical simulation at the Jacobi simulation center, was a nursing student, he and his classmates regularly volunteered to have their arms poked by a needle in order to facilitate an intravenous drip course. Today for this purpose, nursing schools can use an intravenous trainer, which is a latex arm with replaceable skin and veins.
Working with simulators can keep new doctors from inflicting harm on real patients. During a training session at St. Barnabas Hospital in the Bronx, a student broke five of the manikin's teeth while trying to intubate him, according to Ann Marie McDonald, the trauma program coordinator of the hospital.
In the past 10 years, growing concerns for patient safety and advancements in simulation technology are leading more and more medical schools and hospitals across the U.S. to open up simulation labs.
Would you ever get on an airplane if your pilot says I never did a flight simulator because it's too expensive and I don't believe in it? said Haru Okuda, MD, the executive director of the Jacobi simulation center. It is one of those things I think everyone that walks into a hospital knows it's the right thing to do.
The driving force behind the rise of medical simulation is a report on patient safety published in 1999 by the Institute of Medicine, an independent group that advises the government on health issues.
The report, To Err Is Human, initiated a patient safety movement in the U.S. At least 44,000 people, and perhaps as many as 98,000 people, die in hospitals each year as a result of medical errors that may have been prevented. Even using the lower estimate, preventable medical errors in hospitals still exceed attributable deaths to such feared threats as motor vehicle accidents, breast cancer and AIDS, according to the report.
Although official statistics on exactly how many medical schools and teaching hospitals utilize simulation technology are unavailable, about 27,000 health care providers and emergency medical services nationwide, including 237 in New York City, have purchased medical simulation products from Laerdal Medical Corporation, a major manikin and simulator maker headquartered in Norway with a branch office in New York, said Andrew Tweeddale, the company's data integrity analyst.
Right now there are two major types of simulation products. A partial-task simulator, the less sophisticated of the two, resembles a particular body part, such as an intravenous trainer or an AirSim Bronchi, which represents a head and detailed anatomy of the windpipe, and is used for practicing one specific task like inserting an intravenous drip or intubation. A human body simulator represents a whole body and can replicate many physiological indicators including chest rise, bowel sounds, and a blocked airway.
Traditional medical education has a lot of lecturing and memorizing of arcane terms and theories. Even after students proceed to a residency program, what they do for the most part is still observing others, rather than doing procedures themselves. The emergence of simulation has prompted medical education to shift from knowledge-based practice to competence-based practice, said Errichetti, of the New York College of Osteopathic Medicine.
In the past three to four years, as medical simulation has become more widely used, many institutions have conducted longitudinal studies and published evidence-based papers that demonstrate its effects on patient safety.
A study published in 2008 in Simulation in Healthcare, a prominent journal that covers the field of medical simulation, showed that clinicians that went through simulation training reported various aspects of their teamwork had significantly or somewhat improved as a result of the course either immediately afterwards or a year or more later. Eighty-six percent reported the principles in the course as useful for obstetrics faculty, and 59 percent recommended repeating the simulation course every two years.
The Controlled Risk Insurance Company (CRICO), Risk Management Foundation (RMF) of the Harvard Medical Institutions did the study to reduce malpractice cases in obstetrics, which are the highest paid-out cases in health care, because the injuries are often devastating.
As a result of the study, CRICO/RMF developed a simulation-based team-training course for obstetric clinicians, and made the course a central component of its obstetric risk management incentive program that provides a 10 percent reduction in obstetrical malpractice premiums annually.
Studies done in other fields such as cardiology showed similar positive results. In 2007, Chest, the official journal of the American College of Chest Physicians, published a study done at Northwestern Memorial Hospital in Chicago about whether simulation training can improve the quality of care delivered by cardiac arrest teams.
The targets of the study were second-year and third-year residents at the hospital's internal medicine department. All the residents received traditional cardiac life-support training, but second-year residents participated in extra sessions practicing on a human-patient simulator. The goal of the training was to train qualified physicians that adhere to American Heart Association (AHA) guidelines on cardiac life support.
According to the same study, residents that have gone through simulation sessions showed 68 percent adherence to AHA standards, compared to 44 percent in residents that only received traditional training.
It was fabulous, said Eileen Conde, a midwife team leader from North Central Bronx Hospital who participated in the shoulder dystocia course at Jacobi Hospital. It felt very real, and I actually felt a little nervous.
Conde, 50, said she encountered a shoulder dystocia situation during her first year as a midwife. Fortunately an experienced midwife took over and delivered the baby safely. But I did feel helpless not having the skills at that time, said Conde.
What the experienced midwife did was exactly what she learned that morning. After the delivery, the midwife also went over the steps of how to deal with shoulder dystocia with her. She's a good teacher, said Conde. But back then the experience wasn't hands-on. She described what she did, and I saw what she did, but I didn't do it.
One side of the simulation center operating room has a mirror. Behind the mirror is a control room where technicians can manipulate the things happening under the OR lights. The technicians can run a computer code to make the simulator have a heart attack, or a sudden heart-rate drop, or even a blackout to test the team's emergency reaction and cooperation.
Each simulated training session is recorded for a debriefing afterwards. Doctors and nurses critique each other's performance, and discuss what went well and what needs working on.
Shoulder dystocia does not happen very often, but when it does, it catches you off guard, said Timothy Clapper, PhD, who develops courses at the simulation center. He said many other surgical skills have the same problem, such as establishing a surgical airway, an emergency medical procedure that opens a new airway from the front of the patient's neck, usually done when the patient suffers from severe facial damage and cannot be intubated from the mouth.
These situations are so rare in real-life settings that human patients are not always available for teaching. A doctor's muscle memory may grow rusty without sufficient practice, so simulators offer more opportunities to enhance health providers' skills.
However, the simulators alone cannot improve patient care. Another essential element is a new educational philosophy.
Prior to coming to the simulation center, Clapper had a 20-year career in the Army, where he was involved in military simulation of combat operation and evacuation of wounded people. In the military, you practice like your life depends on it, said Clapper. In the medical world, it's the same thing.
Clapper pursued professional degrees in education after his military career. He is not a trained clinician, but he said this is exactly why he should teach at the simulation center. Because I don't assume things, Clapper said.
He explains every little detail to the learners here. A very simple procedure, washing hands before touching sterilized materials, can remarkably reduce the in-hospital infection rate, but many doctors and nurses forget to do this when things begin to whip by rapidly. So before every session, Clapper mentions this step until it becomes second nature.
They already know the skills when they come here, said Clapper. But these skills are not yet solidified in clinical settings, and they don't have the team roles and communication skills.
Clapper sees himself as a facilitator nurturing a desire for knowledge and promoting an active learning process. Traditional teachers, who lecture and encourage rote learning, still dominate many health-care institutions with simulation technology. A teacher may talk about the procedures using PowerPoint slides, and then the students proceed to another room and perform the procedure by themselves. This is not the best way to maximize the use of simulation, he said.
On that Tuesday morning, the simulation class actually began at 9:30 in the meeting room. Ten obstetrics health care providers gathered there for a didactic course intended to introduce them to the theories.
Clapper divided them into two groups according to their roles, so that every group had a mix of attending physicians, nurses and midwives.
We have a Vegas rule here, said Clapper. Everything that happened in this room stays in this room. I want to create a safe learning environment.
He told his students that during an obstetrics emergency, it's common for everyone to try and help, without anyone taking leadership and effectively communicating with other team members. That's a time waster.
Everybody says 'let me try it' and then maneuvers the baby for a few minutes, but totally it's eight or nine minutes past, said Clapper.
He asked his students to write down the consequences and complications of shoulder dystocia on the white board.
After the brainstorming process, students received topic sheets explaining different aspects of the shoulder dystocia condition. You should start getting loud here, Clapper said, encouraging them to talk about the things they do not understand with group members first.
After the group discussion he briefly went over the technical material such as internal maneuvers, and how to deliver the arm first to make the baby's body narrower. Then he talked about communication skills.
Anybody here can be the leader, because you are empowered to be, he said. Talk to your teammates, and let them know what's going on. He also encouraged them to boost mutual support by saying I got your back or We went through that simulation class together.
After the talking, he and Kutzin each led a group of students to practice the new teamwork skills on a part-task trainer that only resembles a woman's hip and thighs. After the rehearsal, they went into the operating room where Elsie gave birth.
Right now the classes at the simulation center focus on surgical skills training, because these are the most critical issues facing hospitals, and hybrid simulation, a more complex form of simulation that involves both simulators and human actors, still represents a very small portion of the training.
A novel use of simulation is to incorporate it into residency program interviews. At St. Barnabas Hospital in the Bronx, applicants to this year's general surgery residency program were asked to do teamwork with a simulator and then confront family members played by professional actors.
In the simulation lab at St. Barnabas, a group of applicants surrounded a TraumaMan simulator, which resembles an adult man's torso. Robert Scott Bostwick, the lab manager, explained the scenario: This man was hit by a train; he has multiple facial lacerations and he cannot breathe; his mental status is poor.
Then he typed on a computer to make the simulator's heart rate and blood pressure appear on the monitor.
Each applicant within the group took the trauma team leader role once, and talked everybody else through the process of establishing surgical airways, inserting chest tubes or other trauma life-support procedures needed.
After the simulator trial, the applicants had to disclose bad news to relatives played by professional actors.
In one scenario, the applicant must explain to the patient's mother that he needs a blood transfusion. The mother is a Jehovah's Witness, whose religion forbids such procedures, and she became hysterical at the prospect. At the end of each session, the actor scores the applicants on how comfortable each physician made her feel.
Ian Eaton, a professional actor who has appeared on TV shows like Law and Order, was one of the actors involved in the interview process. I just don't want to be judged, Eaton said about his criteria. I want to deal with someone who is competent, smart, friendly and professional.
This is the first year that St. Barnabas Hospital added simulation to the interview process. Applicants don't perform any surgical tasks on the simulator, because this is what the program is going to teach them, explains Vic Vernenkar, MD, the residency program director. The simulation is useful in revealing the applicants' ethical standards and communication skills.
We used to have 40 applicants with the same impressive results, said Dr. Vernenkar. How are we going to differentiate? He said there were many candidates that looked very promising on the transcript and recommendation letters, but just perform badly as surgical residents.
The applicants did not shy away from the program because of this extra step. I do think it was a good assessment of a person's character and leadership skills, said Olabisi Ogunro, 26, a student from the University of North Texas' Health Science Center. It is a better evaluation than the traditional transcripts. Many applicants said they enjoyed the simulation lab part, and thought their performance was good.
So far St. Barnabas Hospital is the only New York hospital that is doing this. Most still rely on a resume and transcript, an interview and several recommendation letters to make their selections.
In November, the New England Journal of Medicine published a study led by Dr. Christopher P. Landrigan, an assistant professor at Harvard Medical School, who found that preventable medical errors such as bleeding and infection are still prevalent in U.S. hospitals.
The study showed that about 18 percent of patients were harmed by hospital care, some more than once, and 63.1 percent of the injuries were preventable, and 2.4 percent of the problems caused or contributed to the patients' death.
I believe 100 percent that simulation is going to help improve patient care outcomes, said Dr. Okuda. But it's a piece of it, you can't do it without other things in place like changing culture, changing attitudes, putting guidelines; there are all these tools that are out there, and one by itself is not going to improve.
Kutzin, the director of nursing and clinical simulation at the Jacobi center, said a concern within the nursing profession about simulation is that some nursing schools count the time spent in a simulation lab toward clinical hours required for graduation. I think the opportunity to actually interact with patients, and experience the real clinical setting needs to be preserved, he said. It's important to go onto the floors and learn about the environment you are going to practice in.
Medical simulation cannot solve all the challenges facing the medical and nursing professions, but it does offer an unprecedented way of learning.
The use of simulation wherever feasible conveys a critical educational and ethical message to all: patients are to be protected whenever possible and they are not commodities to be used as conveniences of training, writes Amitai Ziv, the first author of the paper, Simulation-Based Medical Education: An Ethical Imperative, who is also the director of the Israel Center for Medical Simulation.
Shortly after her simulation class, Dr. Connell encountered a patient with a shoulder dystocia emergency. She did exactly what she did during the simulate scenario, applying the maneuvers and calling for help. I felt much more comfortable applying maneuvers, she said. The nurses who were assisting her had gone over the simulation class as well, so everybody was calm and knew what to do. That's a good thing, Dr. Connell said.
© Copyright IBTimes 2024. All rights reserved.