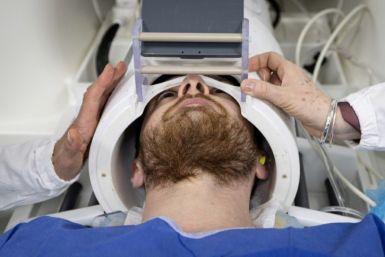
Scientists Claim To Have Found Evidence That Chronic Fatigue Syndrome Has Biological Basis
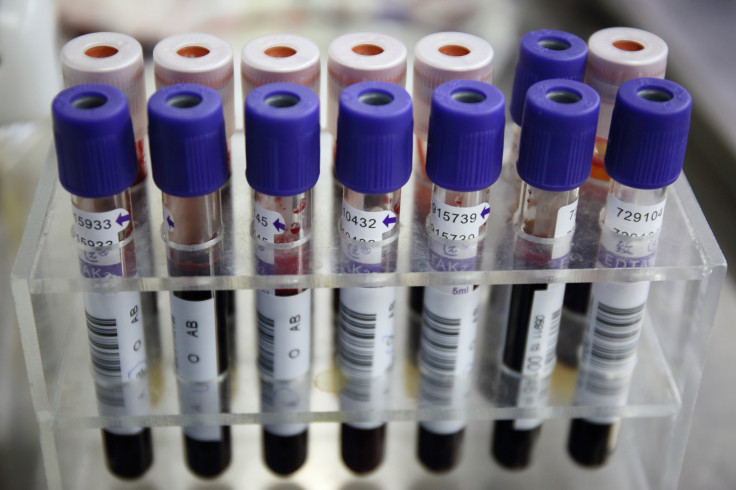
Researchers have found biological evidence for Chronic Fatigue Syndrome (CFS), according to a study published Friday. Although the finding has no clinical applications, researchers say it represents a major step toward developing a diagnostic test for the disease.
CFS, also known as Myalgic Encephalomyelitis (ME), is a mysterious condition which causes severe fatigue, lack of concentration, and sleep disturbances. Classifying the condition has proved controversial, as doctors have argued over whether the condition is psychological or has an underlying physical cause. Friday’s study, if accurate, would be strong evidence in support of a biological basis.
Researchers, led by scientists from Columbia University, published their results in the journal Science Advances. In it, they investigated 51 proteins released by immune system cells called cytokines. They discovered that people who had CFS/ME for less than three years had elevated levels of cytokines compared to control groups and those who had the condition for longer.
“A biomarker has been the goal for much of the research for the last 15 years, so it’s really excellent that they have found something they consider significant,” Dr. Birgitta Evengard, of Umea University in Sweden, told The New York Times. Evengard, who was not involved with the research, cautioned that the findings needed to be replicated before they could be considered certain.
When researchers tested blood samples from 298 patients with ME/CFS, and 348 healthy people, they found no major differences in their levels of cytokines. However, the study then compared cytokine levels in patients who had been sick for less than three years compared to those had been sick longer.
They found that patients who had contracted ME/CFS less than three years ago had significantly higher levels of cytokines that influence inflammation in tissues, and those sick for longer than three years showed dampened cytokine activity, which researchers said might be a sign of a prematurely aged immune system.
Columbia University Professor Mady Hornig, who led the study, said the findings were evidence “confirming what millions of people with this disease already know, that ME/CFS isn’t psychological,” The Independent reported.
The skepticism and lack of awareness surrounding the condition has earned the criticism of several doctors and patients, with the U.S.-based Institute of Medicine calling for more public awareness and medical acceptance of the condition in a report published February, and suggesting the disease be renamed Systemic Exertion Intolerance Disease to better reflect its severity.
“Many healthcare providers are skeptical about the seriousness of ME/CFS, mistake it for a mental health condition, or consider it a figment of the patient’s imagination,” the report said. “The committee stresses that health care providers should acknowledge ME/CFS as a serious illness that requires timely diagnosis and appropriate care.”
© Copyright IBTimes 2024. All rights reserved.