Coronavirus Insurance: Trump Won't Open Obamacare Exchanges To The Suddenly Unemployed
KEY POINTS
- 27 million Americans lacked health insurance before the coronavirus pandemic hit and layoffs have boosted that number by millions
- The administration could have opened a special enrollment period, something sought by insurers and lawmakers
- Those who lost employer-based coverage can still buy COBRA or private plans. Some may qualify for Medicaid
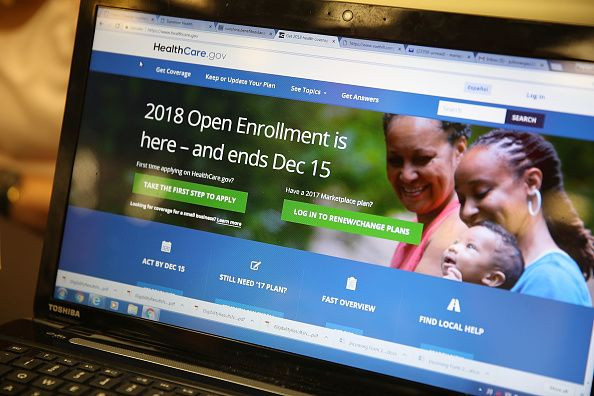
People who have recently lost jobs will not be able to sign up for health insurance through the Affordable Care Act’s Healthcare.gov despite urging from insurers and Congress seeking a special enrollment period amid the coronavirus pandemic.
President Trump said last week the administration was considering a special enrollment period as millions of Americans find themselves unemployed suddenly as a result of the COVID-19 pandemic, which has forced nonessential businesses to close their doors due to social distancing guidelines put in place to slow spread of the infection that has killed more than 44,000 worldwide, more than 4,100 in the United States.
Some 27 million Americans were without health insurance at the end of 2019, before the pandemic hit the U.S. That’s down from 46.5 million in 2010, the year the ACA was enacted.
Current law allows those who have lost job-based insurance coverage to enroll on the marketplaces, but they have to provide proof they have lost coverage. A special enrollment period would have eliminated the proof requirement and allowed people who missed the last enrollment window, which normally runs from Nov. 1 to Dec. 15, to obtain coverage.
Eleven states that control their own marketplaces -- California, Colorado, Connecticut, Maryland, Massachusetts, Minnesota, Nevada, New York, Rhode Island, Vermont, Washington – and the District of Columbia have established their own special enrollment periods.
“This was what the Affordable Care Act is here for,” Sabrina Corlette, head of Georgetown University’s Center on Health Insurance Reforms, told Politico. “The individual market is a true safety net, and that is what it was designed to do -- to catch people in this situation.”
The trade organization, America’s Health Insurance Plans, notes numerous carriers have waived copays and cost-sharing for testing and, in some cases, treatment for COVID-19 infections. AHIP had endorsed reopening the exchanges to help mitigate the costs to both consumers and healthcare providers and urged Congress to expand premium subsidies.
Trump has long worked to overturn the ACA, known as Obamacare, but never came up with any replacement despite promises of better coverage for less money.
“We’re taking care of our people. This is not their fault what happened, and we’re taking care,” he said noting most Americans will get checks for $1,200 from the government as part of the economic relief package signed into law Friday.
“There’s no economic or public health rationale to not open the doors wide in the face of the pandemic,” Peter Lee, the executive director of Covered California, said in opening the state exchange last month.
Americans who had health insurance from their employers can still extend their coverage through COBRA, but that can be a costly proposition. Another alternative, for those who qualify, is Medicaid. And there’s always private coverage.
Politico reported insurers had expected the administration to announce a special enrollment period last week and it was unclear why the administration decided against the move.
As of shortly before noon Wednesday, the U.S. had more than 190,000 confirmed coronavirus infections.
© Copyright IBTimes 2024. All rights reserved.





















