New Study Explores Virus To Fight Superbugs
FDA Legally Warned On Antibiotics Use in Farm Food
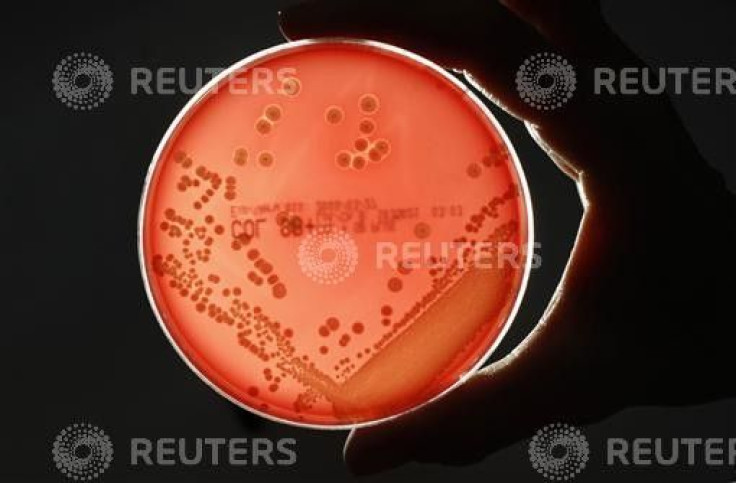
The advent of highly resistant bacteria or superbugs was one of the issues discussed at the Society for General Microbiology's Spring Conference currently being held in Dublin between 26-29 March. An important aspect of the meet was to bring forth new research that focused on combating the advent of superbugs or drug-resistant bacterial strains.
A logic proposed was to use viruses called bacteriophages to wipe out bacterial strains that are resistant to the current crop of antibiotics. The growing menace of accelerated antibiotic resistance has added to the woes of the medical fraternity in combating bacterial diseases that remain resistant to existing antibiotics.
This has reduced the number of potent antibiotics for treating drug-resistant diseases. The novel bacteriophage therapy could be the answer to the growing superbug malady. New research has re-investigated the characteristics of bacteriophages as the potential killer virus that has the ability to infect drug-resistant bacteria by multiplying within the bacterial cells and breaking them down.
In the process, the virus itself enhances its own inner mechanism to deal better with other bacterial strains. The bacteriophages are widely present in the environment such as rivers, water, soil, the human body and sewage. The new idea is to tap these viruses.
Each bacteriophage is highly specific to a certain type of bacteria and needs the right bacterial host cell in order to multiply. The more bacterial targets there are, the quicker they grow by killing the host cells. Therefore it seems very likely that infections harboring high numbers of bacteria will benefit most from bacteriophage therapy - for example chronically infected ears, lungs and wounds, explained Dr. David Harper at the the Dublin meet. He is the Chief Scientific Officer at AmpliPhi Bioscience, Bedfordshire, that has conducted clinical trials on bacteriophages since 2005.
For these types of infection, only a tiny dose of the virus is needed - as small as one thousandth of a millionth of a gram. This can usually be administered directly to the site of infection in a spray, drops or a cream. The major advantage to bacteriophages is that they don't infect human cells so seem likely to be very safe to use, Harper added.
Bacteriophages, discovered initially in 1915, were seen as mere anti-bacterial therapeutic agents but a lack of understanding on their mode of action failed to pave the way for future investigations as anti-bacterial agents. With the advent of new-age chemical variants of anti-bacterial drugs, the viral impact on bacteria remained ignored.
The rate of new antibiotics coming onto the market does not match the rate of increasing drug-resistance. The need for new approaches to counter such high resistance is both urgent and vital. New approaches will save lives, added Harper.
Harper is positive on the results of clinical trials and said that once regulatory issues are taken care of and enough funds are generated to secure this area of research on bacteriophages, the development of the novel viral-based antibacterial agents would be a step to curb the prevailing crisis of drug-resistant antibiotics.
FDA Warned On Antibiotic Use On Farms
In a proactive stance, the Food and Drug Administration (FDA) has received a legal diktat to act on its 35-year-old ruling, aimed at farmers to avoid using popular antibiotics in preparing animal feed. The FDA's 1977 directive was to minimize the ever increasing crisis of drug-resistant bacteria.
The recent ruling called last Thursday directed the FDA to initiate steps in banning approval given to two antibiotics that are used routinely in animals. The ruling was in conjunction with consumer safety groups that brought a lawsuit against the FDA. Public health advocates had been putting pressure on the federal government to restrict the use of antibiotics in farms that has lead to difficulty in treating diseases caused by drug-resistant bacteria.
The FDA has 60 days to appeal to the legal ruling. Although the new court ruling will not impact the use of antibiotics instantly, it has been left to the FDA to enable drug firms to respond and schedule a public hearing.
The FDA had called for a ban on the non-medical use of penicillin and tetracycline in farm animals unless they were proven to be absolutely safe. Farming lobbies have often argued that antibiotics are essential to keep livestock and poultry healthy. This argument has been disputed by food producers who rely on natural resources to keep their cattle disease-free.
FDA's directive was never enforced due to strong resentment from members of the Congress and from lobbyists representing both farmers and pharmaceutical companies. The FDA ruling was based on a 1977 study that inferred that overuse of antibiotics in livestock damaged the potency of these drugs against bacterial-infections in humans.
A recent FDA estimate states that nearly 80 percent of all antibiotics sold in the US are administered on farm animals used in food production.
© Copyright IBTimes 2024. All rights reserved.











