As Theranos Presses Pause, The Real Healthcare Revolution Is Happening With Artificial intelligence, 3D Bio-Printing and Smart Drugs
LONDON -- Theranos and 23andMe promised so much. These well-funded startups' game-changing services -- blood tests available at your local Walgreens and health-risk indicators given from a sample of your saliva -- seemed to usher in the era of personalized and instant healthcare a few years ago. But with Theranos now pressing pause on the development of its proprietary technology and 23andMe continuing to fight the U.S. Food and Drug Administration to let it provide customers with health risk information, the bright future they heralded seems to be on hold.
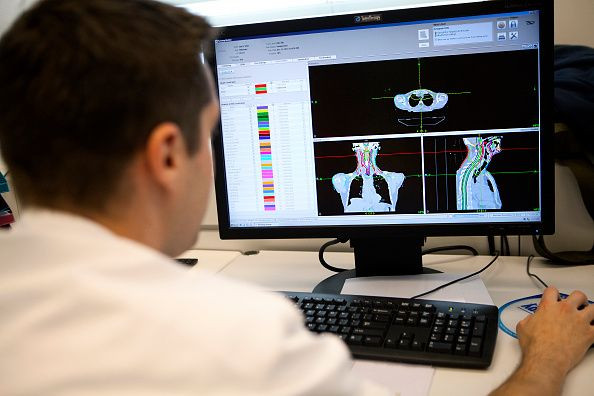
Until you hear about all the other companies, mostly unknown, offering radical changes in the way the healthcare systems work. They are using techniques like 3D bio-printing, artificial intelligence (AI) and smart drugs to predict diseases before they develop, tailoring treatments to individuals rather than the general population and, theoretically at least, providing the tools that could let us live forever.
“Microsoft allowed every family in the world to participate in personal computing. Apple allowed the world to communicate in very different and dynamic ways. My hope and my humble dream is to allow everybody to participate in their own health," said Niven Narain, the co-founder, president and chief technology officer at Berg, a Boston-based company using AI to create smart, tailored treatments that work for specific patients in half the time it traditionally takes and at a fraction of the cost.
Berg is just one of a group of companies at the forefront of a revolution promising to fix what Narain calls a “completely broken” system, and that revolution is already happening. “The shift is not about to come, or the paradigm is not about to change: It has changed. We are in the middle of it,” Narain told International Business Times in London after he spoke at the Wired 2015 conference.
One-Size-Fits-All Approach
Everyone has seen the headlines proclaiming "revolutionary drug breakthroughs" and "positive results from life-saving drug trials" only for that promise to evaporate or for the drug to take years to come to market. Indeed the healthcare startup landscape is littered with big bets and corresponding failures.
The problem at the heart of the healthcare industry is the way drugs are developed. It can take up to 15 years for a drug to reach consumers, and that process can cost $2.5 billion in research and development. The current one-size-fits-all approach to drug development means that for every 100 drug candidates that reach the first-stage clinical trials, only one makes it into the hands of patients. Last year pharmaceutical companies spent $50 billion on research and development, but the FDA approved only 40 new drugs. “In any other industry in the world, we would all be fired,” Narain said dryly.
Big Pharma is facing an impending patent cliff, which Narain says will see 60 percent of revenues disappear by 2017 as patents on the biggest-earning drugs run out. With biotech stocks falling sharply in recent months, companies like AstraZeneca, Pfizer, Roche, Novartis and others are looking over their shoulders at the companies looking to take their place.
This Is The Future
His company brings together AI, big data and precision medicine to comb through vast troves of information about specific patients to find out which treatment works best for them. This approach has allowed them create a drug for pancreatic cancer -- currently in testing -- which can identify reactivate mitochondria in dying cells, preventing them from becoming cancerous. This approach is to take data from the patient's tissue, use proprietary algorithms to create a map of what is causing the disease and point researchers in the direction of a specific treatment.
Those identified with metastatic pancreatic cancer have an average life expectancy of just six months and it is one of the toughest versions of the pernicious diseases to treat -- with Narain saying that 90 percent of patients failing the first line of therapy. Berg's approach is only made possible through the use of AI, and Narain believes this is the way all drugs will soon be developed:
"If you are developing drugs that are biology based, and you have an artificial platform to help match your patients to drugs, this is the future," Narain says. And the system works. The company has reduced the time it takes to discover a viable drug candidate, which typically takes between three and five years at a cost of $150 million, to less than 12 months, and while Narain wouldn’t reveal the exact cost, he did tell IBT the cost was less than half what is normally spent on this process.
Shortening the time it takes to identifying ideal candidates for drug trials is just the first hurdle the industry needs to overcome.
Printing Human Tissue
With drugs needing to go through a series of clinical trials before getting FDA approval, one of the main sticking points is the switch from testing on animals to human trials, with up to 50 percent of drugs failing to make it past this point. Organovo, a 3D bio-printing company, says it can make a big difference here, by printing human tissue and using that as an additional checkpoint in the drug-development process between animal and human trials.

“What works for the animal often doesn’t work for the human,” said founder and chief scientific officer Gabor Forgacs, “So before we go to the human organ, why don’t we try something on the level of a printed tissue and eventually we will be able to eliminate animal trials.”
Organovo has sparked a lot of hype and in September it saw its shares rise more than 55 percent before settling back down again. The reason for the roller-coaster stock price is down to the fact that while the potential impact of Organovo’s technology is huge, it is far from guaranteed.
Some have jumped years ahead by predicting the technology will lead to the 3D printing of organs, but Forgacs is quick to dampen such enthusiasm. “Even if this is possible, it is going to take a long time, so don’t smoke too much, don’t drink too much, because we are not yet there.”
With cutting-edge technology like this, there is always the chance that the promise is never realized. Forgacs is eager to highlight what is possible today, which is the ability to bio-print small livers which are architecturally and functionally correct, and pharmaceutical companies are using those tissues already for toxicity tests, allowing for patient-specific tests by using the patient’s own cells -- which will eventually help the development patient-tailored drugs.
The near future, according to Forgacs, will see the creation of model organisms by putting together those engineered tissues -- liver, kidneys, etc -- which will allow companies like Berg test and develop drugs on this artificial system. A potentially even more critical use for this technology would be as a stop-gap in the organ donation process, using small 3-D-printed organs to keep terminal patients alive until a donor is found. In the U.S. alone in 2014 over 120,000 people were on the organ donor waiting list, with less than 25,000 of those receiving the organs they needed to stay alive, which highlights just how important Organovo’s technology could be.
Your AI Nurse
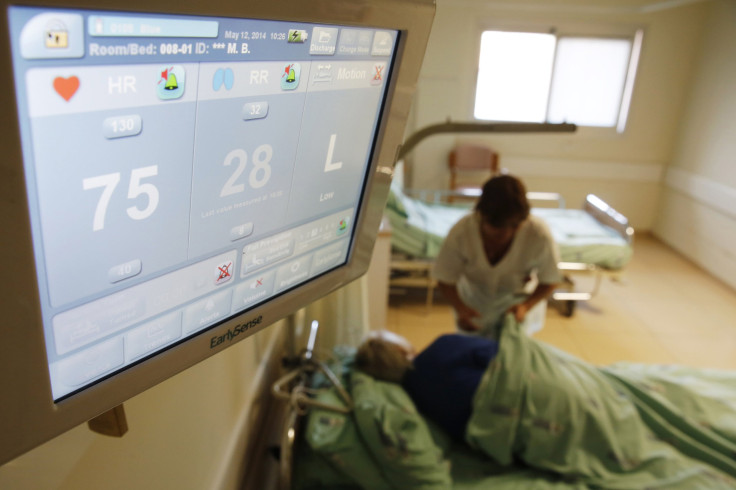
Organovo's technology may be used to limit the damage of disease, but another technology company is already using its cutting-edge techniques to prevent the diseases ever developing. Sentient Technologies, the world’s most well-funded AI company, is using the world’s most powerful AI network to create a new type of nurse, one which predicts when a patient might develop a disease with incredible accuracy. In the word’s of Sentient’s founder Antoine Blondeau, it is developing a nurse that is ”always on the clock, always on the lookout for you, monitoring your vitals at any given time, preempting problems.”

To highlight the potential of this technology, Sentient partnered with the Massachusetts Institute of Technology, to build a system that would specifically address the problem of the blood disease sepsis. Sepsis is the single biggest problem intensive care units (ICUs) have to deal with, affecting 1 million people each year in the U.S. alone, with a mortality rate between 28 and 50 percent - - that’s higher than prostate cancer, breast cancer and AIDS combined. Add to this the fact that sepsis costs ICUs $20 billion every year, and it is clearly a problem that needs to be addressed.
Working with St. Michael’s Hospital in Toronto, Sentient learned that if doctors were given a 30-minute warning that sepsis was coming, they would be able to treat the problem. After a year of collecting arterial blood pressure data “beat by beat” from 6,000 patients, they set their AI nurse to work; it was able to predict the onset of sepsis with over 91 percent accuracy.
“We are using artificial evolution to solve problems brought about by our own biological evolution. The good thing about artificial evolution is that it doesn’t take billions of years to solve problems. We can solve it in days, weeks, months,” Blonde said.
Reaching The Limits Of Our Ability
On Wednesday, 23andMe was granted a license by the FDA to begin offering customers in the U.S. health data again. The company’s founder Anne Wojcicki told IBT ahead of the FDA’s decision, that part of the reason it got shut down in the first place was naivety. “I think what happened is that we reached the limits of our ability and we didn’t have a very experienced team on the regulatory side, [but] we now have an incredibly experienced team and I think we understand much better now all the things we did not know.”
While 23andMe's main attraction for the user is the ability to get genetic information about their ancestors as well as their potential risk of developing a certain disease, the big opportunity for the company is in the data which is it collecting. Wojcicki says the company has the world's biggest pool of genetic information with over 80 percent of its userbase -- which recently passed the one million mark -- agreeing to that data being used for drug development.
While 23andMe is carrying out some of the research itself, it is also generating revenue from companies like Pfizer and Genentech who pay for access to the data. This is the new reality of the pharmaceutical industry where the big giants of the industry know they need to address the "broken" system of drug development, and look at what companies like Berg are doing.
Emotive
Narain says he knows companies like Roche, Novartis and AstraZeneca are all making moves in the AI area already and hiring non-traditional employees like mathematicians. With AI such a hot topic in a wide variety of industries at the moment, the big problem for companies will be hiring the right people, with “everyone hired two or three years before they finish their degrees” according to Narain, meaning there is unlikely to be a stable jobs market in the AI field for five to seven years.

Healthcare is a hugely emotive subject, and one that people feel passionately about. The negative press which Theranos and 23andMe have attracted recently could potentially delay people's willingness to adopt the use of cutting edge technology. Narain however disagrees, seeing the work companies like Berg, Sentient and Organovo are doing, as completely different:
“I think it is separate because their business model is using the samples to perform a test, a sequence and the issues that come up are privacy and prediction. What we are doing is showing the disease exists and predicting, of the folks that have the disease, how you are going to respond.”
The regulators have also changed their tune of late says Narain, and are now asking for "molecular adaptive trials" meaning the stumbling blocks preventing this new way of developing drugs from accelerating are disappearing. Add to this the U.S. government's $215 million pledge precision medicine genetics plan announced by President Barack Obama in January, and a similar scheme in the U.K. called Genomic England, which 23andMe is taking part in, and it appears as if officials want tbi revolution to happen as much as those driving it.
Nothing Preventing Us Living Forever
So just how far could this technology take us? Forgacs, who wanted to become a medical doctor when he was young but says he chickened out because he fainted at the sight of blood, may say he is eager to play down the potential of Organovo's 3=D bio-printing technology, but in the same breadth is happy to show us a vision of the future where he has found the fountain of youth.
"As bizarre as it might sound, there is not theoretically proven limit to longevity," said Forgacs. "We could live forever. We don’t because we are like an automobile and have parts, and those parts get worn off, and eventually we disappear. But what if we could indeed replace our organs with the bio-printed ones?"
This future, if it is even possible, is still a long way off but so too, says Blondeau, is another potential stumbling block when it comes to the general public embracing this technology. Elon Musk and Stephen Hawking may warn us of the potential danger of AI, but Sentient's CEO says we are nowhere near that point:
"I do not believe for one second that what we are doing or what others are doing in the industry is dangerous. We are not there yet. It will take a long time for this to become this out-of-control science fiction stuff."
© Copyright IBTimes 2024. All rights reserved.





















