How The South Can Save The World From Pandemics
The COVID-19 pandemic has confirmed in the most lethal terms that we live in a connected world. No region on the planet has been spared the impact of the virus, with its worldwide death toll exceeding 1.5 million. By now, everybody has heard of the Chinese city of Wuhan and its live animal market that triggered the cataclysmic spread of a disease, which, more than a year after its first detection, is finally seeing its first vaccine distributions.
In Wuhan, one brave doctor sought to raise the alarm early, but his warnings were unheeded. The worst health and economic crisis in a century could have been avoided if only we had a system that empowers regional solutions to combat diseases. Instead, the world suffers from a flawed top-down paradigm where developed economies dominate the means for the control of viruses, particularly in the development and distribution of vaccines.
To beat COVID-19 and to prevent new pandemics, the world needs a boots-on-the-ground strategy of detection and prevention in all the regions of the globe, including the poor as well as the rich. More than a quarter of the world's population lives in Africa and Latin America alone. Rather than remaining neglected, these people in the Global South must be empowered to stop the next outbreak from spreading from a city in the Amazon to the streets of Tokyo.
The prevention of a pandemic begins with early local detection, quick responses to these warnings in the very areas where they first emerge, and ends with providing tailor-made vaccines that can halt the virus in its tracks.
Sadly, the current system of developing vaccines centrally in developed economies and then deploying them globally ensures delayed distribution to regions with the most urgent need. The longstanding pharmaceutical practice of research and development risks failure. Scientists from France to the United States cannot properly take into account local factors such as supply chain capabilities, local environment and population characteristics, especially if they are faced with a mutating virus.
Solutions in the South
Instead, the world should foster the capacity in the South to develop, produce, test and distribute vaccines. This will not only be cost-effective, it will be more effective at stopping the spread. It would also contrast with current plans to combat COVID-19.
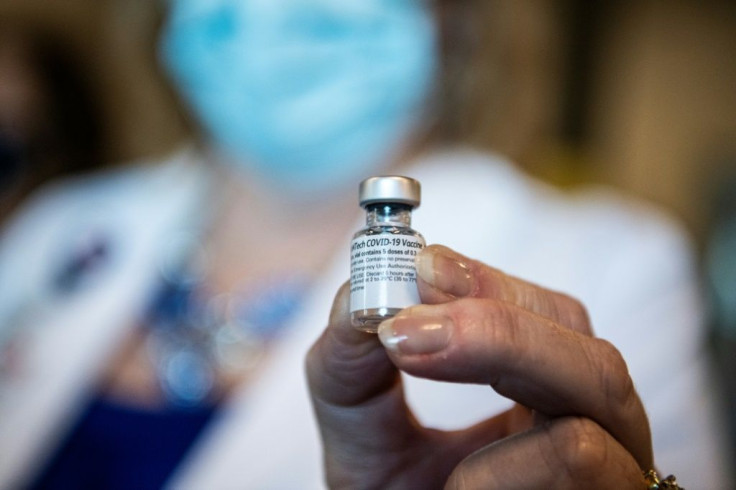
In spite of global efforts through COVAX and similar initiatives, people in poorer countries are set to be some of the last to receive the vaccines that have been developed in rich countries. In addition, even when vaccines do arrive, the complex, cumbersome logistics will overwhelm the infrastructure in poorer countries. The first vaccine, developed by Pfizer, has to be transported at extreme cold temperatures. This prompted Brazil's health ministry to dismiss the chance of distributing the life-saving medicine within Latin America's largest country.
Besides, the first wave of vaccines all require two doses to be effective, but large parts of the population in rural areas (which are a significant percentage of the total in Africa) have to walk long distances to get access to each dose. For COVID-19, we need a second wave of vaccines that are better suited to protect the realities of people living in the poorer South. We also need attention to diseases that mostly affect the South, such as dengue fever and others.
Ready and willing
The good news is that much of the groundwork needed to combat disease has already begun in the South. Over the last few years, Latin America and Africa have set up outstanding capabilities in terms of human resources of excellence to face pandemics. Several countries in South America and in Africa have developed ecosystems to support in-place developments aimed at responding to different goals in human health.
Indeed, the scientific response to the current pandemic resulted in the development of kits for molecular and serological screening. Vaccines are being developed under different platforms that might be used not only for the current crisis but for future pandemics too. While COVID-19 has hit poorer economies hard, all these capabilities remain in place and are ready to join global anti-pandemic efforts.
Beyond the current situation, new global challenges will emerge. It is hard to predict what they will be. It may be a mutation of the virus that causes COVID-19 making current vaccines ineffective; or a new virus that passes from animals to humans; or the next time, the origin could be a distant village in Mozambique, or a crowded mega-city in Latin America. Whatever and wherever this next threat begins, the world must be better prepared. A more distributed global network all the way from detection, development, manufacturing and distribution would be a step in the right direction.
(Santiago Kraiselburd is the CEO of Vaxinz, a biotechnology company that focuses on human infectious and neglected diseases in Africa, Latin America and the Caribbean.)
© Copyright IBTimes 2025. All rights reserved.





















