Opioid Addiction: What Happens During Drug Overdose, How To Stop It
Opioid addiction and abuse is one of the biggest health issues facing the United States, with many health officials and advocates referring to the situation as an “opioid crisis” or the “opioid epidemic.” But the situation keeps getting worse.
The Centers for Disease Control and Prevention notes that drug overdose deaths are rising in the U.S., with more than 60 percent of them linked to opioids. The numbers of opioid prescriptions and overdoses from opioids have both roughly quadrupled since 1999 and about 90 people in this country die from an opioid overdose every day. Here’s what you need to know about these drugs and their effects.
What is an opioid?
Opioids are drugs that bind to your brain cells’ opioid receptors — which normally connect with natural body chemicals like endorphins — to reduce pain. They also activate a feeling of pleasure in the brain, which gives people the feeling of being high.
Although the illegal drug heroin is closely associated with opioid abuse, there are prescription opioids as well that can be addictive and might be abused. Those include Oxycontin, Vicodin, Percocet, Dilaudid, Demerol, codeine, Percodan and morphine-based drugs, among others. There is also the synthetic opioid painkiller fentanyl, which is much more potent and thus potentially more deadly.
Signs of opioid addiction
According to the Mayo Clinic, people who abuse opioid painkillers might have physical symptoms such as slowed breathing, confusion and drowsiness. They might also exhibit changes in behavior — they may steal or otherwise seek prescriptions, take more than the prescribed dose of the drug, have trouble sleeping and display mood swings and risky behavior. People who are addicted to painkillers could have strained relationships and their work or academic performance could suffer.
What happens during an opioid overdose
People who are overdosing on an opioid, whether it be heroin or a prescription painkiller, will be unconscious, have depressed breathing and have pinpoint pupils, according to the World Health Organization. The U.S. Substance Abuse and Mental Health Services Administration warns to call 911 if the victim is pale, clammy and limp; has purple or blue fingernails and lips; and is vomiting or making gurgling sounds.
How to stop an overdose
The most effective way to stop an overdose is to prevent it from happening at all, by working to curb an addiction or getting help for a loved one who needs it. But those are not options when someone is in the middle of an overdose and needs immediate help. For those situations, when someone has a close friend or relative who is battling addiction and might need a medical rescue at some point, there is an anti-overdose medication that saves lives.
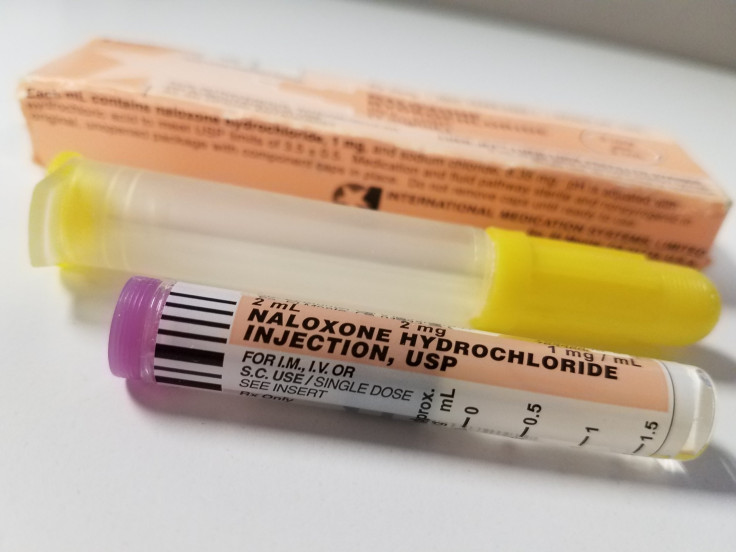
Naloxone (brand name Narcan) is a drug that “binds to opioid receptors and can reverse and block the effects of other opioids,” the U.S. National Institute on Drug Abuse explains. “It can very quickly restore normal respiration to a person whose breathing has slowed or stopped as a result of overdosing with heroin or prescription opioid pain medications.”
It does not have an effect on people who are not overdosing on opioids.
This rescue drug is available in different forms — as an intravenous injection, as an injection into the thigh or as a nasal spray. Although all three have been made available to the public with training, the nasal spray is the most widely shared with people who are not medical professionals. Different states have different rules about who can acquire naloxone, although it is available with a prescription in most of them. In some areas, police departments or volunteer ambulance groups may provide workshops in which professionals train the public to use naloxone and provide them with free kits that include doses of the medicine. There are also certain drug stores that in many states will sell naloxone without a prescription.
60 Minutes has reported that the situation has gotten worse as congressmen and the pharmaceutical industry worked to make it easier for drug distributors to disburse opioids to pharmacies and hospitals.
© Copyright IBTimes 2025. All rights reserved.





















