Why Is Syphilis Making A Comeback?
Syphilis is a sexually transmitted disease (STD) that was nearly eradicated in the U.S., and many doctors haven’t seen a case in years. But following a spike recent reports, the disease appears to be making a comeback.
Cases of syphilis rose nearly 20 percent between 2014 and 2015, the last year data is available, according to the Center for Disease Control and Prevention (CDC). That rate outpaced other STDs like Gonorrhea and Chlamydia. The reason for the increase is a complicated mesh of factors that include increased drug use, lapsed attention and lack of funding.
Earlier this year, Oklahoma declared a syphilis outbreak because of one of the largest infection increases in state history. It was also one of the largest in the country, according to the New York Times Thursday.
“I've worked in STD services for about 13 years now, and we've never been able to connect this many cases to any infection and to an outbreak. It's the largest that I've seen,” Kristen Eberly, who works for Oklahoma’s health department, told the Tulsa World in March.
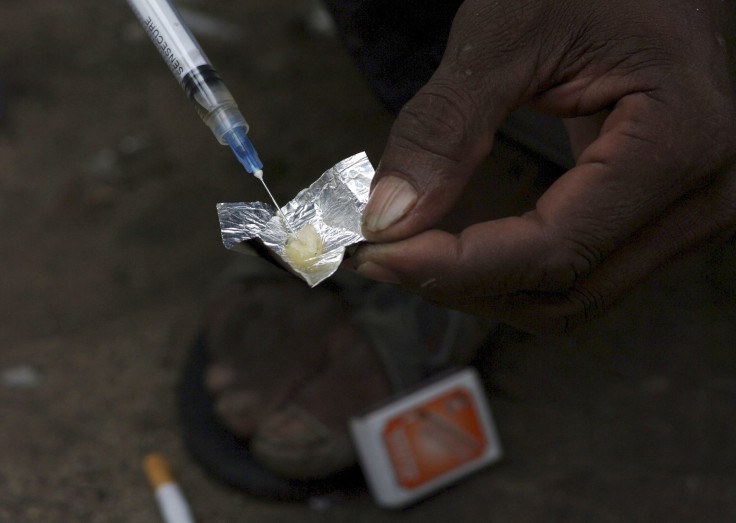
The outbreak was tied to reverberations of the opioid crisis. The most at-risk population was drug users, specifically of heroin or meth. Heroin users can transmit the disease because of sharing needles dirty with the blood of another user. Also, people who exchange sex for drugs are at risk if they have multiple at-risk partners or often inadequate precautionary protection like condoms.
Though the disease still mostly affects gay and bisexual men who are black and Hispanic, rates are rising among white women and infants, according to the CDC.
Syphilis, though curable, is also really hard to detect. The disease’s nickname is the “great pretender,” because its symptoms are often confused with other diseases. Many doctors and nurses have not treated a case since the ‘90s — or ever for newer medical professionals — leading to misdiagnosis. Often the disease can lay dormant before showing symptoms or symptoms will not appear at all. Patients treated and cured of the disease may always show up as positive in testing.
Oklahoma, like many other states, experienced a shortage in the treatments this year, at one point only having seven available. The treatment consists of two injections and is only made by Pfizer.
Funding for treatment and prevention has also been reduced. More than half of all state and local budgets for STD programs saw a reduction in 2012, according to the CDC. This means there have been fewer STD screenings, prevention measures taken and hours for health clinics to be open. At least 21 clinics closed altogether.
And more cuts may come. President Donald Trump has proposed lowering the prevention budget 17 percent.
“We need to improve our screening and treatment,” said Gail Boldan, director of the Division of STD Prevention at the CDC, to USA Today in July. “And we need our communities to realize syphilis is back. They think it’s an ancient disease, but people need to realize this is a significant health problem.”
© Copyright IBTimes 2025. All rights reserved.





















