Eczema Genetic Testing In At-Risk Infants Could Be Possible Soon
KEY POINTS
- Scientists identified and observed gene variations that cause eczema
- Researchers found lower KIF3A protein in mice caused by increased skin water loss
- Genetic testing could help identify infants at risk of developing eczema
A new study has determined the variations in the gene called KIF3A that cause atopic dermatitis or eczema. This discovery could be the key to identifying and protecting the infants that are at risk of developing the skin condition.
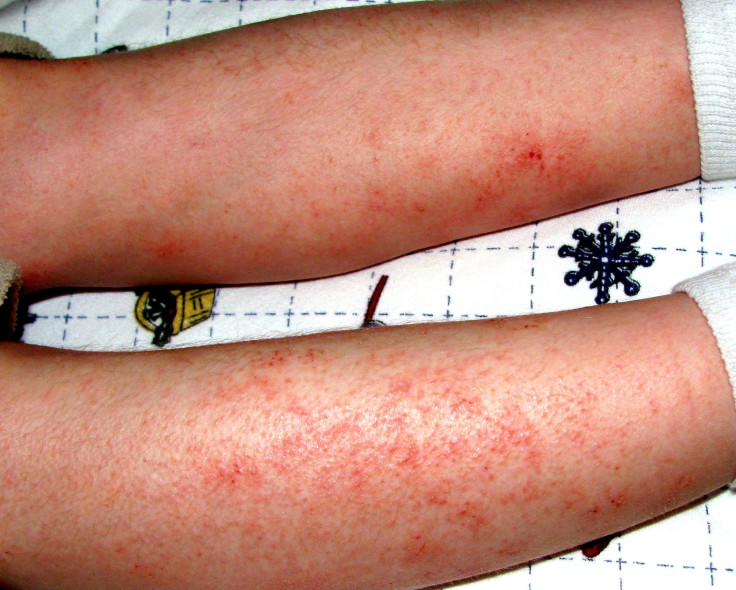
Eczema is an inflammatory skin disease characterized by the drying of the skin. It is an itchy condition, so most people who have it tend to scratch their skin. Aggressive scratching could cause irritated skin to release clear fluid. Although non-contagious, the National Institute of Allergy and Infectious Diseases reported that about 30% of the U.S. population struggle with atopic dermatitis.
To this day, the cause of eczema is still unknown. But medical scientists have resolved that a combination of genetic and environmental factors is responsible for the development of the condition. Between the two, genetics has more weight since children whose parents have history of asthma and allergies tend to develop the skin disease.
In the new study published in the journal Nature Communications, researchers revealed that they have found and delineated the two variations of the gene KIF3A that are responsible for the impairment of the skin barrier, which regulates water loss, causing atopic dermatitis to develop.
The variations, or single nucleotide polymorphisms (SNPs), that the team led by Mariana L. Stevens observed were said to have been altered through a process called methylation. The increase in methylation activity caused the production of the KIF3A protein to dip and the regulating sites in the skin and nasal-lining cells to not function properly. As such, higher levels of water loss in the skin became inevitable.
Stevens, who is associated with the Cincinnati Children’s Hospital Medical Center’s Division of Asthma Research, and her colleagues conducted an experiment on mice to find out if the lower levels of the mouse equivalent of the KIF3A protein would really cause a problem in the skin barrier. They found out that the mice who had more SNPs did manifest increased water loss from the skin.
The findings of the study could propel scientists to come up with genetic tests that could be used in screening infants that are at higher risk of developing atopic dermatitis. Therapies targeting water loss from the skin due to the SNPs to prevent eczema in early childhood could also be developed from here on out, according to the National Institutes of Health.
© Copyright IBTimes 2025. All rights reserved.





















